

Volume 29, Issue 2 (Spring 2023)
Intern Med Today 2023, 29(2): 73-80 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Mardaneh J, ُSharifimood F, Ahmadi R, Zendehdel S, Nemati Shahri F, Mohammadzadeh A. Investigating the Variation in Antibiotic Resistance Pattern in Bacteria
Isolated from Patients with Nosocomial Infection in Allameh Bohlool Gonabadi
Hospital from 2017-2020. Intern Med Today 2023; 29 (2) :73-80
URL: http://imtj.gmu.ac.ir/article-1-4001-en.html
URL: http://imtj.gmu.ac.ir/article-1-4001-en.html
Jalal Mardaneh1 

 , Farnoosh ُSharifimood2
, Farnoosh ُSharifimood2 

 , Reza Ahmadi3
, Reza Ahmadi3 

 , Sorour Zendehdel4
, Sorour Zendehdel4 

 , Fatemeh Nemati Shahri5
, Fatemeh Nemati Shahri5 

 , Alireza Mohammadzadeh *6
, Alireza Mohammadzadeh *6 




 , Farnoosh ُSharifimood2
, Farnoosh ُSharifimood2 

 , Reza Ahmadi3
, Reza Ahmadi3 

 , Sorour Zendehdel4
, Sorour Zendehdel4 

 , Fatemeh Nemati Shahri5
, Fatemeh Nemati Shahri5 

 , Alireza Mohammadzadeh *6
, Alireza Mohammadzadeh *6 


1- Department of Microbiology, School of Medicine, Infectious Diseases Research Center, Gonabad University of Medical Sciences, Gonabad, Iran
2- Department of Internal Medicine, School of Medicine, Infectious Diseases Research Center, Gonabad University of Medical Sciences, Gonabad, Iran
3- Department of Internal Medicine, School of Medicine, Infectious Diseases Research Center, Gonabad University of Medical Sciences, Gonabad, Iran.
4- Student Research Committee, School of Medicine, Gonabad University of Medical Sciences, Gonabad, Iran
5- Microbiology Laboratory, School of Medicine, Gonabad University of Medical Sciences, Gonabad, Iran
6- Department of Microbiology, School of Medicine, Infectious Diseases Research Center, Gonabad University of Medical Sciences, Gonabad, Iran ,alm13604@gmail.com
2- Department of Internal Medicine, School of Medicine, Infectious Diseases Research Center, Gonabad University of Medical Sciences, Gonabad, Iran
3- Department of Internal Medicine, School of Medicine, Infectious Diseases Research Center, Gonabad University of Medical Sciences, Gonabad, Iran.
4- Student Research Committee, School of Medicine, Gonabad University of Medical Sciences, Gonabad, Iran
5- Microbiology Laboratory, School of Medicine, Gonabad University of Medical Sciences, Gonabad, Iran
6- Department of Microbiology, School of Medicine, Infectious Diseases Research Center, Gonabad University of Medical Sciences, Gonabad, Iran ,
Full-Text [PDF 644 kb]
(978 Downloads)
| Abstract (HTML) (3500 Views)
Nosocomial infections are recognized as one of the most daunting challenges posed to healthcare centers due to their great contribution to increased mortality, disability, length of hospitalization, and treatment costs. According to the World Health Organization (WHO), nosocomial infections refer to those occurring within 48 hours of hospital admission, 3 days of discharge, or 30 days of an operation [1]. According to the WHO report, one out of every 20 hospitalized patients suffers from nosocomial infection. These infections cause or contribute to 99,000 deaths each year, imposing a high cost of 26-32 million dollars on society [2, 3]. Various factors are involved in increasing the risk of nosocomial infections, including underlying disease, disease severity, length of hospitalization, and invasive devices, such as ventilators and urinary catheters [2].
Surveys by the WHO in different regions of the world demonstrated that 5%-25% of patients admitted to hospitals suffer from nosocomial infections. This rate has been reported as 25% in the intensive care unit (ICU) in developed countries and up to 50% in developing countries. Therefore, the risk of nosocomial infections in patients hospitalized in the ICU is 5-7 times higher than that in general wards [4]. Furthermore, according to the studies conducted, the overall prevalence of these infections in Iran is reported to be 4.6% [5]. Nosocomial infections are mainly caused by pathogenic bacteria, such as Klebsiella pneumonia, Staphylococcus aureus, Escherichia coli, Pseudomonas aeruginosa, and Proteus [6].
The amount and type of nosocomial infection vary across different hospitals and medical centers; nonetheless, urinary infections, surgical site infections, respiratory infections, and infections of the circulatory system account for more than 80% of nosocomial infections [7]. Antimicrobial resistance is the ability of microorganisms to survive in the presence of antimicrobial substances at concentrations usually sufficient to inhibit or kill them. Currently, available antibiotics are less effective on microorganisms, and the development of new strategies is essential for their management [8]. Bacterial resistance exhibits different mechanisms, such as modifying the antibiotic's target by the bacteria, inactivating bacterial enzymes, reducing drug permeability, and expelling the antibiotic from inside the cell [9, 10].
Studies conducted around the world indicate that nosocomial infections are mainly caused by antibiotic-resistant organisms. Antimicrobial resistance is a naturally occurring process. Nonetheless, factors, such as inappropriate and excessive use of antibiotics, indiscriminate access to antibiotics, and a failure to monitor their use are among the most important reasons for the marked increase in drug-resistant bacteria [5]. Today, the emergence of new mechanisms of microbial resistance has turned into one of the most serious challenges that threaten human health in the modern era. Moreover, the ongoing spread of multidrug-resistant bacteria has raised a global concern, which has led to an increase in mortality rates and healthcare costs. Moreover, the spread of multidrug-resistant strains has restricted the treatment methods effective for infectious diseases [11].
Antimicrobial resistance aggravates nosocomial infections, reduces the effectiveness of antibiotics, and increases healthcare costs, treatment duration, and mortality [12, 13]. Nosocomial infections are one of the serious health and treatment problems presented to every country, contributing to the death of numerous hospitalized patients every year; moreover, antibiotic resistance is increasing among patients with nosocomial infections. Therefore, assessing the epidemiology of nosocomial infections and their antibiotic resistance patterns is a practical step in controlling these infections in the hospital and reducing mortality and treatment costs. To the best of our knowledge, no study has been conducted in this regard in Gonabad; therefore, the present study aimed to assess the variation in the antibiotic resistance pattern of bacteria isolated from patients with nosocomial infection in Allameh Bohlool Gonabadi Hospital from 2017-2020.
Table 1. Demographic characteristics of patients
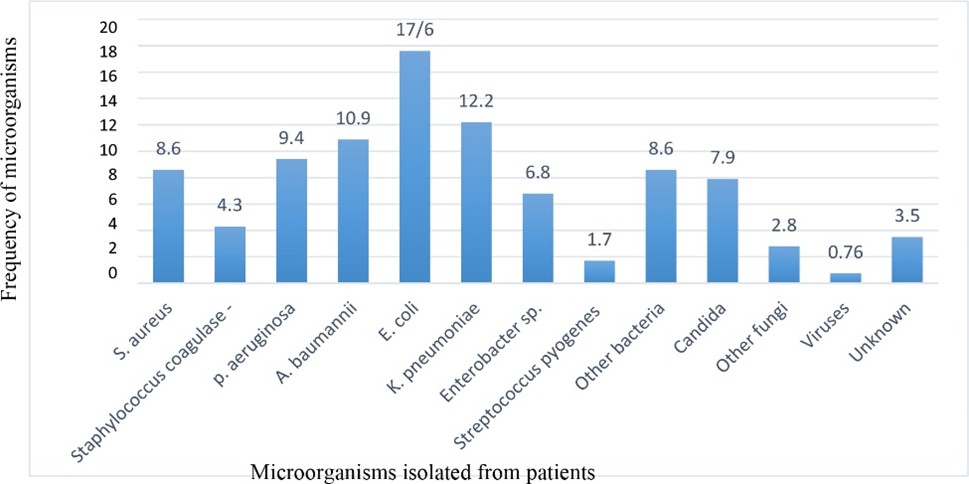
Figure 1. Frequency of microorganisms isolated from patients
Table 2. Antibiotic resistance of bacteria isolated during 1997-2020

Figure 2. Comparing the frequency of multidrug-resistant bacteria by year
Full-Text: (562 Views)
|
Nosocomial infections are recognized as one of the most daunting challenges posed to healthcare centers due to their great contribution to increased mortality, disability, length of hospitalization, and treatment costs. According to the World Health Organization (WHO), nosocomial infections refer to those occurring within 48 hours of hospital admission, 3 days of discharge, or 30 days of an operation [1]. According to the WHO report, one out of every 20 hospitalized patients suffers from nosocomial infection. These infections cause or contribute to 99,000 deaths each year, imposing a high cost of 26-32 million dollars on society [2, 3]. Various factors are involved in increasing the risk of nosocomial infections, including underlying disease, disease severity, length of hospitalization, and invasive devices, such as ventilators and urinary catheters [2].
Surveys by the WHO in different regions of the world demonstrated that 5%-25% of patients admitted to hospitals suffer from nosocomial infections. This rate has been reported as 25% in the intensive care unit (ICU) in developed countries and up to 50% in developing countries. Therefore, the risk of nosocomial infections in patients hospitalized in the ICU is 5-7 times higher than that in general wards [4]. Furthermore, according to the studies conducted, the overall prevalence of these infections in Iran is reported to be 4.6% [5]. Nosocomial infections are mainly caused by pathogenic bacteria, such as Klebsiella pneumonia, Staphylococcus aureus, Escherichia coli, Pseudomonas aeruginosa, and Proteus [6].
The amount and type of nosocomial infection vary across different hospitals and medical centers; nonetheless, urinary infections, surgical site infections, respiratory infections, and infections of the circulatory system account for more than 80% of nosocomial infections [7]. Antimicrobial resistance is the ability of microorganisms to survive in the presence of antimicrobial substances at concentrations usually sufficient to inhibit or kill them. Currently, available antibiotics are less effective on microorganisms, and the development of new strategies is essential for their management [8]. Bacterial resistance exhibits different mechanisms, such as modifying the antibiotic's target by the bacteria, inactivating bacterial enzymes, reducing drug permeability, and expelling the antibiotic from inside the cell [9, 10].
Studies conducted around the world indicate that nosocomial infections are mainly caused by antibiotic-resistant organisms. Antimicrobial resistance is a naturally occurring process. Nonetheless, factors, such as inappropriate and excessive use of antibiotics, indiscriminate access to antibiotics, and a failure to monitor their use are among the most important reasons for the marked increase in drug-resistant bacteria [5]. Today, the emergence of new mechanisms of microbial resistance has turned into one of the most serious challenges that threaten human health in the modern era. Moreover, the ongoing spread of multidrug-resistant bacteria has raised a global concern, which has led to an increase in mortality rates and healthcare costs. Moreover, the spread of multidrug-resistant strains has restricted the treatment methods effective for infectious diseases [11].
Antimicrobial resistance aggravates nosocomial infections, reduces the effectiveness of antibiotics, and increases healthcare costs, treatment duration, and mortality [12, 13]. Nosocomial infections are one of the serious health and treatment problems presented to every country, contributing to the death of numerous hospitalized patients every year; moreover, antibiotic resistance is increasing among patients with nosocomial infections. Therefore, assessing the epidemiology of nosocomial infections and their antibiotic resistance patterns is a practical step in controlling these infections in the hospital and reducing mortality and treatment costs. To the best of our knowledge, no study has been conducted in this regard in Gonabad; therefore, the present study aimed to assess the variation in the antibiotic resistance pattern of bacteria isolated from patients with nosocomial infection in Allameh Bohlool Gonabadi Hospital from 2017-2020.
Materials and Methods
In this descriptive cross-sectional study, the medical files of 392 patients with nosocomial infections hospitalized in Allameh Bohlool Gonabadi Hospital from 2016-2019 were examined. Based on the study by Akbari et al. [14] and considering the significance level of 95% and the acceptable error of 0.05, the required sample size was calculated at 380 cases using the following formula:
This research was approved by the Regional Research Ethics Committees of Gonabad University of Medical Sciences (IR.GMU.REC.1399.074). Patients with nosocomial infections (patients who develop infections 48-72 hours after hospitalization, three days after discharge, or 30 days after surgery) who had a complete medical file were recruited in this study, and patients with incomplete file information were excluded from the study. The required information was extracted from the patient's medical files and recorded on relevant checklists. This information included age, gender, hospital ward, length of hospitalization, bacterial species, type of infection, used instrument, and antibiotic resistance pattern (using disk diffusion method and based on CLSI standard) of bacteria isolated from the medical records of patients with nosocomial infection from 2016-2019. Patients with incomplete clinical information were excluded from the study. Subsequently, all data were analyzed in SPSS software (version 21) using mean and standard deviation for quantitative variables with a normal distribution, median and range for quantitative variables with a non-normal distribution, and number and percentage for describing qualitative variables.
This research was approved by the Regional Research Ethics Committees of Gonabad University of Medical Sciences (IR.GMU.REC.1399.074). Patients with nosocomial infections (patients who develop infections 48-72 hours after hospitalization, three days after discharge, or 30 days after surgery) who had a complete medical file were recruited in this study, and patients with incomplete file information were excluded from the study. The required information was extracted from the patient's medical files and recorded on relevant checklists. This information included age, gender, hospital ward, length of hospitalization, bacterial species, type of infection, used instrument, and antibiotic resistance pattern (using disk diffusion method and based on CLSI standard) of bacteria isolated from the medical records of patients with nosocomial infection from 2016-2019. Patients with incomplete clinical information were excluded from the study. Subsequently, all data were analyzed in SPSS software (version 21) using mean and standard deviation for quantitative variables with a normal distribution, median and range for quantitative variables with a non-normal distribution, and number and percentage for describing qualitative variables.
Results
In this study, a total of 392 patients with nosocomial infection were included, out of whom 173 (44.13%) cases were male and 219 (55.87%) subjects were female. Most patients (52.80%) were seniors (those 65 and older), and the prevalence of nosocomial infections was 0.88%. In this study, the ICU had the highest rate of nosocomial infection among other hospital units, and 183 (46.68%) patients were hospitalized in the ICU. During the study years, ventilator-associated pneumonia (32.14%) was the most common form of nosocomial infection, followed by urinary tract infection (27.55%) and surgical site infection (20.15%). In this study, the mean length of hospitalization (admission to discharge) was 26.4 days (Table 1).
In this study, gram-negative bacilli were the most common causative agents of hospital infection, among which Escherichia coli (17.60%), Klebsiella (12.20%), and Acinetobacter (10.90%) were the most dominant pathogens. Staphylococcus aureus (8.60%) was the most abundant gram-positive cocci isolated from nosocomial infections. In 90.7% of patients, Candida, and in 2.80% of patients, other fungi were identified as the causative agents of nosocomial infection (Figure 1).
In this study, gram-negative bacilli were the most common causative agents of hospital infection, among which Escherichia coli (17.60%), Klebsiella (12.20%), and Acinetobacter (10.90%) were the most dominant pathogens. Staphylococcus aureus (8.60%) was the most abundant gram-positive cocci isolated from nosocomial infections. In 90.7% of patients, Candida, and in 2.80% of patients, other fungi were identified as the causative agents of nosocomial infection (Figure 1).
Table 1. Demographic characteristics of patients
| Year | 2017 n (%) |
2018 n (%) |
2019 n (%) |
2020 n (%) |
2017-2020 n (%) |
| Gender | |||||
| Male | (34.03) 33 | (47.50) 38 | (51.49) 52 | (43.86) 50 | (44.13) 173 |
| Female | (65.97) 64 | (52.50) 42 | (48.51) 49 | (56.14) 64 | (55.87) 219 |
| Age groups | |||||
| 0-4 years | (3.90) 3 | (5.00) 4 | (5.94) 6 | (1.75) 2 | (3.83) 15 |
| 5-14 years (child) | (5.15) 5 | (2.50 )2 | (1.98) 2 | (1.75) 2 | (2.80) 11 |
| 15-24 years old (teenager) | (15.46) 15 | (5.00) 4 | (5.94) 6 | (6.14) 7 | (8.17) 32 |
| 25-44 years old (young) | (11.34) 11 | (17.50) 14 | (15.84) 16 | (15.79) 18 | (15.05)59 |
| 45-64 years old (middle-aged) | (19.59) 19 | (12.50) 10 | (16.84) 17 | (19.03) 22 | (17.35) 68 |
| 65≥ (elderly) | (45.37) 44 | (57.50) 46 | (53.46) 54 | (55.26) 63 | (52.80) 207 |
| Department | |||||
| CCU | (1.03) 1 |
|
(4.95) 5 | (3.50) 4 | (2.56) 10 |
| ICU | (51.54) 50 | (51.25) 41 | (29.70) 30 | (54.39) 62 | (46.69) 183 |
| NICU | (4.12) 4 | (5.00) 4 | (2.97) 3 | (0.87) 1 | (3.06) 12 |
| Pediatric |
|
|
(0.99) 1 | (1.75) 2 | (0.76) 3 |
| Surgery | (24.75) 24 | (17.50) 14 | (25.75) 26 | (10.55) 12 | (19.38) 76 |
| Internal medicine | (18.55) 18 | (25.99) 20 | (34.63) 35 | (22.80) 26 | (25.26) 99 |
| Gynecology | (0)0 | (1.25) 1 | (0.99) 1 | (6.14) 7 | (2.29) 9 |
| Type of infection | |||||
| ventilator-associated pneumonia | (29.89) 29 | (37.50) 30 | (22.77) 23 | (38.59) 44 | (32.14) 126 |
| Pneumonia | (16.49) 16 | (6.25) 5 | (19.80) 20 | (9.65) 11 | (13.27) 52 |
| Urinary tract infection | (26.80) 26 | (32.50) 26 | (24.75) 25 | (27.20) 31 | (27.56) 108 |
| Bloodstream infections | (1.03) 1 | (2.50) 2 | (2.97) 3 | (1.75) 2 | (2.04) 8 |
| Surgical site infection | (22.69) 22 | (13.75) 11 | (23.76) 24 | (19.30) 22 | (20.16) 79 |
| Others | (3.09) 3 | (7.50) 6 | (5.94) 6 | (3.50) 4 | (4.84) 19 |
| Total | 97 | 80 | 101 | 114 | 392 |

The results of this study demonstrated that during the study years, antibiotic resistance displayed an increasing trend among all bacterial isolates, and the highest antibiotic resistance was observed in Acinetobacter, which was resistant to Cotrimoxazole, Ciprofloxacin, ampicillin, meropenem, cefepime, cefazolin, nitrofurantoin, and norfloxacin in 100% of cases. The lowest antibiotic resistance was related to Staphylococcus aureus isolates, 100% of which were sensitive to imipenem, meropenem, and nitrofurantoin.
The antibiotic resistance of E.coli isolates to meropenem gradually increased during the study years. In total, within four years, 100% of E.coli isolates showed resistance to ampicillin, cefazolin, tetracycline, and erythromycin. Klebsiella clinical isolates exhibited maximum resistance (100%) to ampicillin, cefazolin, norfloxacin, erythromycin, and penicillin, followed by ceftriaxone (91.66%) and imipenem (76.83%). Pseudomonas aeruginosa had the highest resistance (100%) to ceftriaxone, cefazolin, and ampicillin, and antibiotic resistance increased in isolates of this bacterium over four years (Table 2).
The frequency of multidrug-resistant isolates by year is illustrated in Figure 2. In total, the most and least abundant multidrug-resistant isolates were Acinetobacter strains and E.coli isolates, respectively. The frequency of multidrug-resistant isolates displayed an increased trend during four years (Figure 2).
The antibiotic resistance of E.coli isolates to meropenem gradually increased during the study years. In total, within four years, 100% of E.coli isolates showed resistance to ampicillin, cefazolin, tetracycline, and erythromycin. Klebsiella clinical isolates exhibited maximum resistance (100%) to ampicillin, cefazolin, norfloxacin, erythromycin, and penicillin, followed by ceftriaxone (91.66%) and imipenem (76.83%). Pseudomonas aeruginosa had the highest resistance (100%) to ceftriaxone, cefazolin, and ampicillin, and antibiotic resistance increased in isolates of this bacterium over four years (Table 2).
The frequency of multidrug-resistant isolates by year is illustrated in Figure 2. In total, the most and least abundant multidrug-resistant isolates were Acinetobacter strains and E.coli isolates, respectively. The frequency of multidrug-resistant isolates displayed an increased trend during four years (Figure 2).
Table 2. Antibiotic resistance of bacteria isolated during 1997-2020
| Bacterium Antibiotics (%) |
Escherichia coli | Klebsiella pneumonia | Acinetobacter baumannii | Staphylococcus aureus | Pseudomonas aeruginosa |
| Cotrimoxazole | 73.81 | 75 | 100 | 25 | 83.3 |
| Ciprofloxacin | 71.15 | 51.2 | 100 | 16.66 | 63.6 |
| Ceftriaxone | 66.44 | 91.66 | 88.88 | 100 | 100 |
| Gentamicin | 69.85 | 48.41 | 66.66 | 50 | 45.5 |
| Amikacin | 58.5 | 47 | 83.33 | 100 | 60.5 |
| Trimethoprim | 66.66 | 50 | 85 | 100 | 100 |
| Meropenem | 62.77 | 50 | 100 | 0 | 75 |
| Imipenem | 70.73 | 76.83 | 91.66 | 0 | 33.3 |
| Tetracycline | 100 | _ | 100 | _ | _ |
| Norfloxacin | 75 | 100 | 100 | 100 | 100 |
| Nitrofurantoin | 38.63 | 66.66 | 100 | 0 | 57.1 |
| Clindamycin | - | - | - | 50 | _ |
| Cefazolin | 100 | 100 | 100 | 75 | 100 |
| Ampicillin | 100 | 100 | 100 | 100 | 100 |
| Ceftazidime | 50 | 50 | 100 | 40 | 66.6 |
| Cefepime | 66.66 | 67 | 100 | _ | 80 |
| Erythromycin | 100 | 100 | _ | 80 | _ |
| Penicillin | _ | 100 | _ | 100 | _ |

Figure 2. Comparing the frequency of multidrug-resistant bacteria by year
Discussion
The present study aimed to assess the variation in antibiotic resistance patterns in pathogens isolated from patients with nosocomial infections admitted to Allameh Bohlool Gonabadi Hospital from 2017-2020. According to the obtained results, the prevalence of nosocomial infections was 0.88%, which is relatively low. In a meta-analysis study by Mosadegh Rad, the prevalence of nosocomial infection in Iranian hospitals was reported between 0.32% and 9.1% [15]. In this regard, the rate of nosocomial infection was estimated at 2.7% in Amir Al-Momenin Hospital in Tehran, 1.7% in a military hospital in Tehran, and 3.06% in Kamkar Hospital in Qom [18-16]. The low rate obtained in our study can be attributed to the failure to identify some people with nosocomial infections or some patients acquiring these infections after being discharged from the hospital.
In general, factors, such as the number of people admitted to the hospital, the type of disease, the size of the hospital, the number of beds, the specialty of the hospital, and the type of services provided in the hospital can affect the prevalence of nosocomial infections [15]. The highest frequency of infections in the present study was observed in the age group over 65 years old (52.8%). Factors, such as a weak immune system, various underlying diseases, and prolonged hospital stay, make this age group more susceptible to nosocomial infections [19].
In the present study, infection caused by a ventilator was the most common form of nosocomial infection, followed by urinary tract infection and surgical site infection (32.4%). In the meta-analysis study by Mosadegh Rad, urinary tract infections, followed by respiratory infections, were reported as the most common type of nosocomial infection in Iranian hospitals [15]. In the study conducted by Darvishpour, surgical site infection, pneumonia, and urinary tract infection were reported as the most common forms of nosocomial infections [20]. Consistent with the results of most studies, In this research, the highest rate of nosocomial infection was related to ICU [21, 22].
Similar to other studies, in this research, E. coli was revealed to be the most dominant pathogen [23-27]. In the present study, the rate of variation in antibiotic resistance patterns in common microorganisms was investigated over four years, and it was observed that the microbial resistance and frequency of multidrug-resistant strains had an increasing trend during the study years. These data are in agreement with other reported results regarding the constant increase of antimicrobial resistance, especially among gram-negative bacteria, in different regions across the globe [28, 29].
Based on the results of the present study, E. coli demonstrated maximum resistance to ampicillin, cefazolin, and norfloxacin and the lowest resistance to nitrofurantoin and amikacin. In the last year of the study, this bacterium was most sensitive to nitrofurantoin, which is clinically valuable. These findings are in line with the results of other studies [13, 30, 31]. During this four-year study, a significant increase was observed in the antibiotic resistance of E. coli strains to meropenem. This finding can be regarded as a warning against excessive use of this antibiotic.
The results of the present study pinpointed that the maximum antibiotic resistance was observed to ampicillin, cefazolin, and norfloxacin in the clinical isolates of Klebsiella as the second dominant pathogen causing nosocomial infections. In addition, consistent with the results of the studies conducted by Samadzadeh and Barak, the lowest antibiotic resistance was related to amikacin and gentamicin [32, 33]. somewhat consistent with some studies, in the present research, Pseudomonas aeruginosa isolates had maximum resistance (100%) to norfloxacin, cefazolin, ceftriaxone, and ampicillin [13, 32, 33]. Nonetheless, contrary to the present research, in the study by Shahraki et al. in Zahedan [34], ceftazidime was suggested as the main option in the treatment of Pseudomonas aeruginosa infections, while in the present study, 100% of Pseudomonas aeruginosa isolates were resistant to ceftazidime.
Acinetobacter clinical isolates exhibited high resistance to most antibiotics except gentamicin. These findings are largely similar to those reported in other studies [13, 35, 36]. In accordance with the findings reported by Pooladi, in the present research, multidrug-resistant Acinetobacter isolates had a higher frequency than other isolates [36]. Among the notable limitations of this study are the retrospective nature of the study, the insufficient accuracy of information based on records, and the incompleteness of information regarding the culture of some isolates. In brief, the significant increase in antibiotic resistance among isolates causing nosocomial infections in recent years is a dire warning for us. It is suggested to exercise great caution when using resistant antibiotics and periodically check the antibiotic resistance pattern of strains. Moreover, to prevent multidrug resistance, it is recommended to refrain from indiscriminate use and prescription of antibiotics prior to antibiograms.
The present study aimed to assess the variation in antibiotic resistance patterns in pathogens isolated from patients with nosocomial infections admitted to Allameh Bohlool Gonabadi Hospital from 2017-2020. According to the obtained results, the prevalence of nosocomial infections was 0.88%, which is relatively low. In a meta-analysis study by Mosadegh Rad, the prevalence of nosocomial infection in Iranian hospitals was reported between 0.32% and 9.1% [15]. In this regard, the rate of nosocomial infection was estimated at 2.7% in Amir Al-Momenin Hospital in Tehran, 1.7% in a military hospital in Tehran, and 3.06% in Kamkar Hospital in Qom [18-16]. The low rate obtained in our study can be attributed to the failure to identify some people with nosocomial infections or some patients acquiring these infections after being discharged from the hospital.
In general, factors, such as the number of people admitted to the hospital, the type of disease, the size of the hospital, the number of beds, the specialty of the hospital, and the type of services provided in the hospital can affect the prevalence of nosocomial infections [15]. The highest frequency of infections in the present study was observed in the age group over 65 years old (52.8%). Factors, such as a weak immune system, various underlying diseases, and prolonged hospital stay, make this age group more susceptible to nosocomial infections [19].
In the present study, infection caused by a ventilator was the most common form of nosocomial infection, followed by urinary tract infection and surgical site infection (32.4%). In the meta-analysis study by Mosadegh Rad, urinary tract infections, followed by respiratory infections, were reported as the most common type of nosocomial infection in Iranian hospitals [15]. In the study conducted by Darvishpour, surgical site infection, pneumonia, and urinary tract infection were reported as the most common forms of nosocomial infections [20]. Consistent with the results of most studies, In this research, the highest rate of nosocomial infection was related to ICU [21, 22].
Similar to other studies, in this research, E. coli was revealed to be the most dominant pathogen [23-27]. In the present study, the rate of variation in antibiotic resistance patterns in common microorganisms was investigated over four years, and it was observed that the microbial resistance and frequency of multidrug-resistant strains had an increasing trend during the study years. These data are in agreement with other reported results regarding the constant increase of antimicrobial resistance, especially among gram-negative bacteria, in different regions across the globe [28, 29].
Based on the results of the present study, E. coli demonstrated maximum resistance to ampicillin, cefazolin, and norfloxacin and the lowest resistance to nitrofurantoin and amikacin. In the last year of the study, this bacterium was most sensitive to nitrofurantoin, which is clinically valuable. These findings are in line with the results of other studies [13, 30, 31]. During this four-year study, a significant increase was observed in the antibiotic resistance of E. coli strains to meropenem. This finding can be regarded as a warning against excessive use of this antibiotic.
The results of the present study pinpointed that the maximum antibiotic resistance was observed to ampicillin, cefazolin, and norfloxacin in the clinical isolates of Klebsiella as the second dominant pathogen causing nosocomial infections. In addition, consistent with the results of the studies conducted by Samadzadeh and Barak, the lowest antibiotic resistance was related to amikacin and gentamicin [32, 33]. somewhat consistent with some studies, in the present research, Pseudomonas aeruginosa isolates had maximum resistance (100%) to norfloxacin, cefazolin, ceftriaxone, and ampicillin [13, 32, 33]. Nonetheless, contrary to the present research, in the study by Shahraki et al. in Zahedan [34], ceftazidime was suggested as the main option in the treatment of Pseudomonas aeruginosa infections, while in the present study, 100% of Pseudomonas aeruginosa isolates were resistant to ceftazidime.
Acinetobacter clinical isolates exhibited high resistance to most antibiotics except gentamicin. These findings are largely similar to those reported in other studies [13, 35, 36]. In accordance with the findings reported by Pooladi, in the present research, multidrug-resistant Acinetobacter isolates had a higher frequency than other isolates [36]. Among the notable limitations of this study are the retrospective nature of the study, the insufficient accuracy of information based on records, and the incompleteness of information regarding the culture of some isolates. In brief, the significant increase in antibiotic resistance among isolates causing nosocomial infections in recent years is a dire warning for us. It is suggested to exercise great caution when using resistant antibiotics and periodically check the antibiotic resistance pattern of strains. Moreover, to prevent multidrug resistance, it is recommended to refrain from indiscriminate use and prescription of antibiotics prior to antibiograms.
Conclusion
As evidenced by the results of this study, there was a significant increasing trend in the resistance of isolates to all studied antibiotics during these four years; moreover, the frequency of multidrug-resistant strains was also increasing. Therefore, a thorough knowledge of antibiotic resistance patterns can be of great help to physicians in selecting more appropriate antibiotics for treatment and preventing the development of antibiotic resistance.
Ethical Considerations
Compliance with ethical guidelines
This study was approved by the Regional Research Ethics Committees of Gonabad University of Medical Sciences (IR.GMU.REC.1399.074).
Funding
The financing of this research was done by the Research and Technology Vice-Chancellor of Gonabad University of Medical Sciences.
Authors' contributions
All authors contributed to this research project.
Conflicts of interest
The authors declare that they have no conflict of interest.
Acknowledgments
We are deeply grateful to the director and staff of the Allameh Bohlool Gonabadi Education and Treatment Center for their assistance in this research project.
- Farzianpour F, Bakhtiari A, Mohammadi M, Khosravizadeh O, Mossavi H, Mohseni M, et al. Analysis of nosocomial infections in selected teaching hospitals, Qazvin, Iran. Health. 2014; 6(18): 2425. [DOI: 10.4236/health.2014.618279]
- Cardo D, Dennehy PH, Halverson P, Fishman N, Kohn M, Murphy CL, et al. Moving toward elimination of healthcare-associated infections: a call to action. Infect Control Hosp Epidemiol. 2010; 31(11): 1101-5. [DOI: 10.1086/656912] [PMID]
- Amini N, Rezazadeh A, Khooshemehri G, Amini M, Salehiniya H. Knowledge, attitude and self-efficacy of nursing staff in nosocomial infection in child hospitals of Tehran University of Medical Sciences. Alborz University Medical Journal. 2015; 4(1): 27-34. [DOI: 10.18869/acadpub.aums.4.1.27]
- Sh Mohammad Z. Microbiological factors in burn wound infection in patients hospitalized in Zanjan. 2011; 6 (22): 65-72. [Link]
- Mohammadi M, Vaisi Raiegan A, Jalali R, Ghobadi A, Salari N, Barati H. The prevalence of nosocomial infections in Iranian hospitals. Journal of Babol University of Medical Sciences. 2019; 21(1): 39-45. [DOI: 10.22088/jbums.21.1.39]
- Jain A, Singh K. Recent advances in the management of nosocomial infections. JK Sci. 2007; 9(1): 3-8. [Link]
- Klevens RM, Edwards JR, Richards Jr CL, Horan TC, Gaynes RP, Pollock DA, et al. Estimating health care-associated infections and deaths in US hospitals, 2002. Public Health Rep. 2007; 122(2): 160-6. [DOI: 10.1177/003335490712200205] [PMID] [PMCID]
- Avershina E, Shapovalova V, Shipulin G. Fighting antibiotic resistance in hospital-acquired infections: current state and emerging technologies in disease prevention, diagnostics and therapy. Front Microbiol. 2021; 12: 707330. [DOI: 10.3389/fmicb.2021.707330] [PMID] [PMCID]
- Cerini P, Meduri FR, Tomassetti F, Polidori I, Brugneti M, Nicolai E, et al. Trends in Antibiotic Resistance of Nosocomial and Community-Acquired Infections in Italy. Antibiotics (Basel). 2023; 12(4): 651. [DOI: 10.3390/antibiotics12040651] [PMID] [PMCID]
- Sousa SA, Feliciano JR, Pita T, Soeiro CF, Mendes BL, Alves LG, et al. Bacterial nosocomial infections: Multidrug resistance as a trigger for the development of novel antimicrobials. Antibiotics (Basel). 2021;10(8): 942. [DOI: 10.3390/antibiotics10080942] [PMID] [PMCID]
- Nimer NA. Nosocomial infection and antibiotic-resistant threat in the Middle East. Infect Drug Resist. 2022; 15: 631-9. [DOI: 10.2147/IDR.S351755] [PMID] [PMCID]
- Hormozi SF, Vasei N, Aminianfar M, Darvishi M, Saeedi AA. Antibiotic resistance in patients suffering from nosocomial infections in Besat Hospital. Eur J Transl Myol. 2018; 28(3): 7594. [DOI: 10.4081/ejtm.2018.7594] [PMID]
- Pourkazemi A, Farashbandi H, Balu H. Epidemiological study of nosocomial infections and antibiotic resistance patterns in Guilan. Yafteh. 2019; 21(1): 52-62. [Link]
- Akbari M, Nejad Rahim R, Azimpour A, Bernousi I, Ghahremanlu H. A survey of nosocomial infections in intensive care units in an Imam Reza hospital to provide appropriate preventive guides based on international standards. Studies in Medical Sciences. 2013; 23(6): 591-6. [Link]
- Mosadeghrad AM, Afshari M, Isfahani P. Prevalence of nosocomial infection in Iranian hospitals: a systematic review and meta-analysis. Iranian Journal of Epidemiology. 2021; 16(4): 352-62. [Link]
- Mesgarian M, Zangeneh M, Farhoodi B, Alijani M, Haghani S, Oladi S. Evaluation of patients' characteristics by diagnosing nosocomial infections and its relationship with the rate of antibiotic resistance in Amir Al-Momenin Hospital. Medical Science Journal of Islamic Azad Univesity-Tehran Medical Branch. 2021; 31(2): 241-50. [DOI: 10.52547/iau.31.2.241]
- Sepandi M, Motahari F, Taheriyan M, Hashemi S. Evaluation of the Prevalence of Nosocomial Infections and their Antibiotic Resistance in one of the military hospitals affiliated Army Medical University during 2018-2019. 2021; 7(25): 24-32. [Link]
- Vafaei K, Razaviyan F, Sheikholeslami N. The Epidemiologic Study of One Year Nosocomial Infections in Kamkar Hospital (Qom) 2008:(A Short Report). Journal of Rafsanjan University of Medical Sciences. 2013;12: 319-24. [Link]
- Rodriguez-Acelas AL, de Abreu Almeida M, Engelman B, Canon-Montanez W. Risk factors for health care–associated infection in hospitalized adults: Systematic review and meta-analysis. Am J Infect Control. 2017; 45(12): e149-56. [DOI: 10.1016/j.ajic.2017.08.016] [PMID]
- Darvishpoor K, Rezaei Manesh MR. Prevalence of nosocomial infections and microbial causes in Torbat heydariyeh 9dey educational and clinical hospital in 2012 and 2013. Iranian Journal of Medical Microbiology. 2016;10(1):93-6. [Link]
- Bagheri P. The review systematic and meta analysis of prevalence and causes of nosocomial infection in Iran. Iranian Journal of Medical Microbiology. 2015; 8(4): 1-12. [Link]
- Kohestani SM, Rahmani H, Nourbakhsh S, Habibi F, Vasoukolaei GR. Epidemiology and determine the causes of nosocomial infectioin teaching hospital of Tehran: a cross-sectional study. Hospital. 2019;18(3): 53-61. [Link]
- Nouri F, Karami P, Zarei O, Kosari F, Alikhani MY, Zandkarimi E, et al. Prevalence of common nosocomial infections and evaluation of antibiotic resistance patterns in patients with secondary infections in Hamadan, Iran. Infect Drug Resist. 2020; 13: 2365-74. [DOI: 10.2147/IDR.S259252] [PMID] [PMCID]
- Sadeghzadeh V. The frequency rate of nosocomial urinary tract infections in intensive care unit patients in Shafiieh Hospital, Zanjan. Retrovirology. 2010; 7(1): P93. [DOI: 10.1186/1742-4690-7-S1-P93] [PMCID]
- Zamanzad B, Naseri F. Comparison of the causative bacteria and antibacterial susceptibility pattern of nosocomial and community-acquired urinary tract pathogens in 13-35 years old women, Shahrekord, 2004. Journal of Arak University of Medical Sciences. 2005; 8(4): 23-30. [Link]
- Rodríguez‐Baño J, López‐Prieto MD, Portillo MM, Retamar P, Natera C, Nuño E, et al. Epidemiology and clinical features of community‐acquired, healthcare‐associated and nosocomial bloodstream infections in tertiary‐care and community hospitals. Clin Microbiol Infect. 2010; 16(9): 1408-13. [DOI: 10.1111/j.1469-0691.2009.03089.x] [PMID]
- Hashemi SH, Esna AF, Tavakoli S, Mamani M. The prevalence of antibiotic resistance of Enterobacteriaceae strains isolated in community-and hospital-acquired infections in teaching hospitals of Hamadan, west of Iran. J Res Health Sci. 2013; 13(1): 75-80. [PMID]
- E. Abou Warda A, Molham F, Salem HF, Mostafa-Hedeab G, ALruwaili BF, Moharram AN, et al. Emergence of High Antimicrobial Resistance among Critically Ill Patients with Hospital-Acquired Infections in a Tertiary Care Hospital. Medicina (Kaunas). 2022; 58(11): 1597. [DOI: 10.3390/medicina58111597] [PMID] [PMCID]
- Kaye KS, Pogue JM. Infections caused by resistant gram‐negative bacteria: epidemiology and management. Pharmacotherapy: Pharmacotherapy. 2015; 35(10): 949-62. [DOI: 10.1002/phar.1636] [PMID]
- Sharif M, Nori S. The Frequency and Antibiotic Resistance of Urinary Tract Infection Organisms in Hospitalized Children. Shahid Beheshti Hospital. Kashan 2012-2013. Iran J Infect Dis Trop Med. 2014; 19(65): 47-51. [Link]
- Heidari SE, Heidari M, Doosti A. Epidemiology of urinary tract infection and antibiotic resistance pattern of E. coli in patients referred to Imam Ali hospital in Farokhshahr, Chaharmahal va Bakhtiari, Iran. 2013, 15(2): 9-15. [Link]
- Samadzadeh S, SadeghI A, Sadeghi R, Rahbar M. Study of frequency and causing factors of urinary tract infections in imam khomeini hospital in urmia. Studies in Medical Sciences. 2002; 13(3): 220-7. [Link]
- Barak M, Mamishi S, Siadati A, Salamati P, Khotaii GH, Mirzarahimi M,. Risk factors and bacterial etiologies of nosocomial infections in NICU and PICU Wards of children's medical center and bahrami hospitals during 2008-2009. Journal of Ardabil University of Medical Sciences. 2011; 11(2): 113-20. [Link]
- Shahraki Zahedani S, Jahantigh M, Amini Y. Determining a pattern for antibiotic resistance in clinical isolations of pseudomonas aeruginosa. Tehran University of Medical Sciences Journal. 2018; 76(8): 517-22. [Link]
- Farahani Kheltabadi R, Moniri R, Shajari GR, Nazem Shirazi MH, Musavi SGA, Ghasemi A, et al. Antimicrobial Susceptibility patterns and the distribution of resistance genes among Acinetobacter species isolated from patients in shahid Beheshti hospital, Kashan. KAUMS Journal (FEYZ). 2009; 12(4): 61-7. [Link]
- Poladi I, Delfani S, Soroush S, Soltani M, Rezaei F. Evaluation of antibiotic resistance pattern of Acinetobacter baumannii clinical isolates in Khorramabad hospitals. Yafteh. 2021; 23(3):158-67. [DOI: 10.32592/Yafteh.2021.23.3.14]
Type of Study: Original |
Subject:
Basic Medical Science
Received: 2023/08/21 | Accepted: 2023/03/10 | Published: 2023/03/10
Received: 2023/08/21 | Accepted: 2023/03/10 | Published: 2023/03/10
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |

